How Wireless Uroflowmeters Enable Remote Patient Monitoring

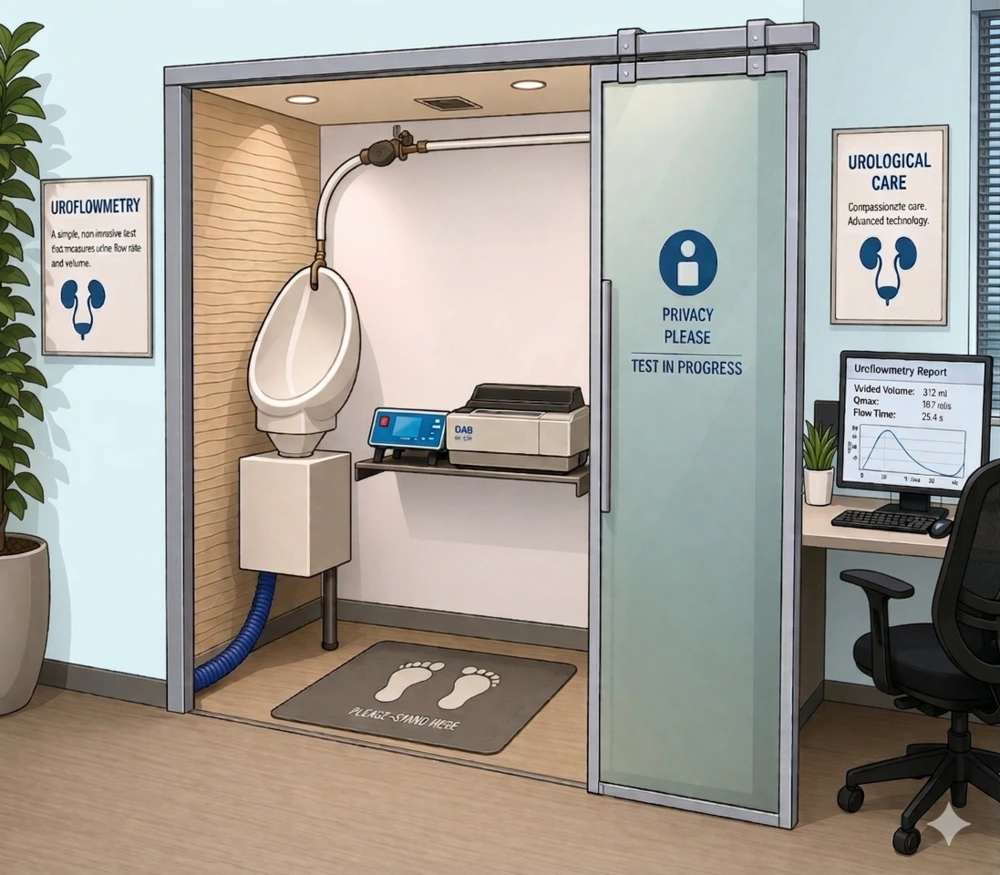
Uroflowmetry is a non-invasive diagnostic test used to evaluate urinary flow and assess patients presenting with lower urinary tract symptoms (LUTS). Wireless uroflowmeters provide objective data on urinary flow, helping clinicians assess bladder function and identify conditions such as bladder outlet obstruction and detrusor underactivity.
In routine clinical practice, however, uroflowmetry is often limited by single measurements taken in controlled environments. These readings may not always reflect the patient’s usual voiding pattern, particularly when symptoms vary or when patient performance is inconsistent.
Wireless uroflowmeters enhance the utility of uroflowmetry by enabling repeated measurements and providing flexible access to patient data within the clinical setting. With connected systems, clinicians can review results remotely without being physically present at the point of testing, making it easier to assess urinary function across multiple sessions.
Clinical Applications of Wireless Uroflowmetry
Wireless connectivity allows clinicians to review and compare uroflowmetry data remotely, supporting continuous patient monitoring beyond a single clinical visit.
| Clinical Scenario | How Wireless Uroflowmetry Helps |
| Borderline Qmax values | Confirms whether reduced flow is consistent across multiple sessions |
| Suspected BPH | Helps identify persistent flow reduction that may not appear clearly in a single test |
| LUT dysfunction | Correlates variable symptoms with objective flow data over time |
| Neurogenic bladder follow-up | Tracks changes in voiding function across repeated measurements |
| Post-treatment monitoring | Compares current results with baseline to assess improvement or stability |
| Functional voiding issues | Captures flow patterns across multiple measurements within the clinical setting, supporting more consistent evaluation of voiding patterns. |
Limitations of Conventional Uroflowmetry
Although uroflowmetry is widely used, its effectiveness can be influenced by the manner and location of the test. In many clinical settings, results are based on a single void, which may not represent the patient’s usual condition.
Factors such as patient anxiety, timing of voiding, and bladder filling can affect results. This often leads to variability, especially in borderline cases where interpretation is not straightforward. Repeating the test under similar conditions is also difficult, limiting the ability to compare results over time. This reduces diagnostic confidence and can delay clinical decisions.
Where Wireless Uroflowmeters Improve Clinical Practice
These wireless uroflowmeters improve clinical practice by enabling repeated measurements under consistent and natural conditions. Their value becomes more evident in situations where a single test does not provide sufficient clarity.
In borderline cases, where peak flow rate is slightly reduced, repeated measurements help determine whether the finding is consistent or influenced by temporary factors. This is particularly useful in early evaluation of conditions such as benign prostatic hyperplasia (BPH), where flow reduction may not always be clearly defined in a single test.
When patient-reported symptoms do not align with initial test results, remote monitoring allows testing at different times and under varying conditions. Wireless uroflowmeters help clinicians better correlate symptoms with objective data, especially in patients with lower urinary tract (LUT) dysfunction, where symptoms and flow patterns may vary.
Role in Follow-Up and Ongoing Monitoring
In follow-up care, repeated testing enables comparison with baseline measurements, supporting more accurate evaluation of treatment outcomes. This is particularly relevant in conditions such as neurogenic bladder, where ongoing monitoring is required to assess changes in voiding function over time.
For functional or behaviour-related voiding conditions, testing within a dedicated patient area in the clinical setting can help create a more comfortable environment. This may reduce variability associated with testing conditions and support more consistent assessment.
Benefits of Wireless Uroflowmeters in Practice
In day-to-day clinical workflows, wireless uroflowmeters improve both diagnostic reliability and operational efficiency. Their ability to support repeated testing and connected data handling makes uroflowmetry more practical in real-world use.
- Repeated measurements help confirm whether reduced flow is consistent across sessions, reducing reliance on single readings.
- Fewer repeat clinic visits improve follow-up compliance, especially in long-term monitoring cases.
- Access to reports across devices makes it easier to review and compare results over time.
- Automated data handling reduces manual errors and supports more efficient workflows.
These improvements make uroflowmetry a more reliable and practical tool for routine clinical use.
Impact on Clinical Decision-Making
The quality of clinical decisions depends on the consistency and reliability of available data. When uroflowmetry is based on a single reading, interpretation may remain uncertain, especially in borderline cases. This provides clinicians with more comprehensive data, helping them make more confident clinical decisions.
Wireless uroflowmeters address this by providing multiple datasets over time. Clinicians can evaluate patterns rather than relying on isolated values, which helps confirm findings and reduces diagnostic uncertainty. This approach is particularly useful for assessing treatment response, as changes in flow patterns can be tracked across sessions to determine whether a patient is improving, stable, or requiring further intervention.
This further supports remote patient monitoring, where clinicians can track changes in urinary flow without requiring the patient to be physically present. As a result, follow-up becomes more consistent and less dependent on clinic visits.
Why Clinics Are Adopting Wireless Uroflowmetry Systems
The adoption of wireless uroflowmeters is largely driven by improvements in both workflow and diagnostic consistency.
- Flexible testing enables uroflowmetry to be conducted in a dedicated patient area while clinicians access data separately, without disrupting the workflow.
- Repeated measurements under similar conditions improve the consistency of results
- Real-time access to patient data supports faster review and clinical decision-making
- Integration with digital systems reduces administrative workload
As a result, wireless uroflowmeters are becoming a practical and scalable solution for modern urology clinics. This enables remote monitoring, allowing clinicians to review patient data without requiring in-person testing for every session.
FlowComp NG Wireless Uroflowmeter
The FlowComp NG Wireless Uroflowmeter is built for everyday use, not just controlled testing environments. It runs on a Wi-Fi system and uses a gravimetric method, meaning flow is measured by weight. That usually gives more stable readings, especially when tests are repeated.
In many clinics, the device is kept with the patient while the clinician checks the results separately. This may seem like a small change, but it can significantly influence how the test is performed. Patients may feel more comfortable during testing when not directly observed, which can help support more natural voiding.
Wireless uroflowmeters work across phones, tablets, and Windows systems. There’s no strict setup required. Reports can be accessed when needed. Comparing previous and current readings becomes a seamless part of routine clinical evaluation.
It’s also fairly simple to use. Most staff don’t need much time to get used to it. And once it’s in place, it doesn’t interfere with the workflow. This ease of use can support smoother clinical operations. This system is designed in accordance with recognised medical device standards and complies with applicable regulatory and safety requirements for clinical use.
Conclusion
Wireless uroflowmeters enhance traditional uroflowmetry by enabling remote monitoring, repeated measurements, and connected data access. Systems like FlowComp NG combine accurate measurement with connected functionality, improving both diagnostic reliability and workflow efficiency.
For urology practices, this means better data, clearer interpretation, and more confident clinical decisions. If you’re relying on single, variable uroflowmetry readings, the FlowComp NG wireless uroflowmeter offers a more consistent, repeatable approach. Contact Status Medical Equipments to learn how it can improve your diagnostic process.
FAQs:
Wireless uroflowmeters are useful in situations where multiple measurements are required to assess urinary flow more consistently. By enabling repeated testing and easier data access, they help clinicians review results across sessions and support more reliable evaluation within routine clinical practice.
Remote monitoring enables tests to be conducted under more natural and consistent conditions. When multiple readings are available, it becomes easier to distinguish between true abnormalities and temporary variations, leading to a more reliable interpretation of flow patterns.
FlowComp NG allows clinicians to review and compare multiple datasets collected over time. This makes it easier to assess whether a patient is responding to treatment and whether changes in flow patterns reflect real improvement or ongoing issues.
Yes. The testing environment can influence results, as factors such as patient comfort and consistency of conditions may affect voiding patterns. Wireless uroflowmeters help address this by allowing testing to be conducted in a dedicated patient area within the clinical setting, improving comfort while maintaining consistent measurement conditions.
Wireless connectivity allows the testing process and data review to happen independently. While the patient completes the test, clinicians can access the data remotely, reducing the need for manual handling and improving overall efficiency.